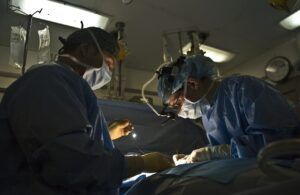
What to Do When You Contract a Hospital-Acquired Infection
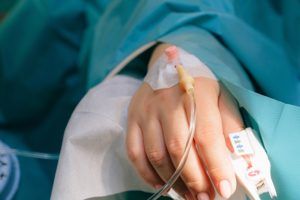
If you or a loved one believes you may have contracted a hospital-acquired infection, here’s what you need to know and what you should do next.
Inadequate care and hospital negligence create unsafe conditions for patients. What’s more, even when hospital staff and doctors do everything right, there is still the potential for something to go wrong with the patient’s care or recovery. One such example is contracting a hospital-acquired infection (aka healthcare-associated infection or “HAI”). There are multiple ways a patient can contract an infection. How the infection plays out will depend on the individual and the type of hospital-acquired infection. If you or a loved one believes you may have contracted a hospital-acquired infection, here’s what you need to know and what you should do next.
What is a Hospital-Acquired Infection?
HAI’s are infections that are not present or might be incubating at the time of admission to a healthcare facility. These infections are often manifest within 48 hours after admission to the hospital. HAI infections include central line-associated bloodstream infections (CLABSI), catheter-associated urinary tract infections (CAUTI), surgical site infections (SSI), Hospital-acquired Pneumonia (HAP), Ventilator-associated Pneumonia (VAP), and Clostridium difficile infections (CDI). 1
T he risk for HAIs is also dependent on the infection control practices at the healthcare facility.
But, as with any infection, the patient’s immune status, and the prevalence of the various pathogens within the community also play a role. For these reasons, it is critical to identify patients with risk factors for HAIs.
What Do I Do if I Think I Contracted an HAI?
First step is to alert your doctor. It doesn’t always take trained medical professionals to identify the signs of hospital-acquired infection. As a patient, if you feel your health condition is not improving, or you have developed new problems, you should immediately alert your doctor. Early detection and treatment can drastically reduce the chances of suffering prolonged effects of the infection. Let the hospital staff know if you experience fever, excessive warmth or pain around a wound, discharge from a wound, headaches, nausea, and any other symptoms causing discomfort.
Recover Damages for the Hospital-Acquired Infection
If you or a loved one suffered an HAI that caused significant harm, i.e. additional medical care, hospitalization, or death, you may be able to file a medical malpractice lawsuit. The experienced medical malpractice attorneys at Cardaro & Peek can review your case to see if you are able to file a claim.
Contact The Law Offices of Cardaro & Peek, LLC Today
Do you believe that you or your loved one has suffered as a result of medical malpractice or medical neglect? You need to talk to an experienced team of local lawyers today.
The lawyers at Cardaro & Peek, LLC have the experience and resources necessary to investigate and litigate all types of medical claims throughout Maryland and Washington D.C. Cardaro & Peek, LLC has medical personnel on staff and has access to nationally recognized, board-certified physicians and other experts, to assist in the investigation, analysis, and prosecution of all types of medical malpractice claims. If you or a loved one have experienced malpractice, give us a call at 410-752-6166. Please visit our website www.cardarolaw.com and follow us on Facebook , Twitter , and LinkedIn for more information.
1 Boev C, Kiss E. Hospital-Acquired Infections: Current Trends and Prevention. Crit Care Nurs Clin North Am. 2017 Mar;29(1):51-65.
The post What to Do When You Contract a Hospital-Acquired Infection appeared first on .